How NewYork-Presbyterian Used Telemedicine to Expand Care in Puerto Rico
Patients in Puerto Rico had access to specialists in Manhattan thanks to peer-to-peer video consultations.


One minute, a young mother was describing her struggles trying to manage her 2-year-old son’s diabetes after Hurricane Maria, recalls Nancy Pagan, a physician assistant and member of NewYork-Presbyterian’s Disaster Response Team in Puerto Rico.
And the next minute?
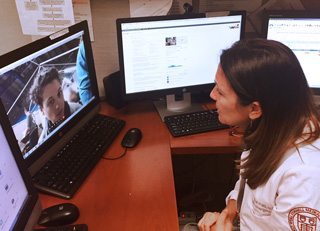
Pagan was consulting with leading specialists in New York about the boy’s care via videoconferencing. Thanks to the launch of a peer-to-peer telemedicine service in Puerto Rico during the time that NewYork-Presbyterian’s team was on the island, patients at a federal medical shelter in Manatí had access to specialists from Weill Cornell Medicine and ColumbiaDoctors through NewYork-Presbyterian’s telehealth service, NYP OnDemand.
“It was wonderful to be able to use telemedicine in Puerto Rico,” says Pagan. “It was a very good feeling to be able to have backup like that in a disaster situation.”
All Pagan had to do was send a text to the doctors and call them up on her computer.
“Once we made the connection, the video worked, the audio worked, and I was speaking to Nancy within a matter of moments,” says Dr. Shari Platt, chief of pediatric emergency medicine at NewYork-Presbyterian Komansky Children’s Hospital and associate professor at Weill Cornell Medicine.
Dr. Platt conducted the telemedicine consultation with Dr. Zoltan Antal, chief of pediatric endocrinology at Komansky Children’s Hospital.
“The beauty of it was that we were able to see the child,” says Dr. Platt. “He was in the background playing and happy. We were able to see that there were no visible complications from diabetes, and we were able to find out what doses of insulin he was on, what his diet had been like, and why he had been running such high sugars.”
“During an emergency, telehealth can play a vital role in providing access to care where it’s needed, and we are so glad that we could extend our service to help those impacted by Hurricane Maria.”— Leo Bodden
Dr. Antal advised adjusting the boy’s insulin dosage to stabilize his blood sugar levels. He encouraged him to return for a checkup. When the boy returned a few days later, “he was doing very well,” Pagan says.
“The ability to bring in the pediatric subspecialties to an environment that otherwise would not have access, that’s a tremendous resource,” says Dr. Platt. “There would be no way to bring all these subspecialists to the disaster center. Telehealth lets our entire department be available.”
The team in Manatí also received adult telemedicine consultations, including advice from an ear, nose, and throat specialist about a patient who had received a tracheostomy.
It was the first time that NewYork-Presbyterian used NYP OnDemand in a disaster-relief situation.
Jeffrey Bokser, vice president of Safety, Security & Emergency Services at NewYork-Presbyterian, says that, with the help of a government agency, they were able to bring in satellite dishes and make telemedicine a reality in just a few days.
“This is something that was very valuable to our providers (on the ground),” Bokser says, “and when you think about emergencies in the future, a real area that we can leverage to best help organizations or responses around the world if we’re called upon to do so.”
“Establishing telehealth via satellite in resource-challenged Puerto Rico is groundbreaking,” says Leo Bodden, vice president and chief technology officer at NewYork-Presbyterian. “During an emergency, telehealth can play a vital role in providing access to care where it’s needed, and we are so glad that we could extend our service to help those impacted by Hurricane Maria.”

