The HIV Epidemic: From Deadly Crisis to Routine Care
For more than three decades, NewYork-Presbyterian’s HIV clinics have worked on the front lines of treating and preventing HIV.
When Drs. Peter Gordon and Samuel Merrick began treating patients at NewYork-Presbyterian’s first HIV clinics more than three decades ago, medicines weren’t effective and people with advanced AIDS were almost certain to die.
“The people I cared for in the early 1990s, most of them passed,” says Dr. Gordon. “Back then, there was little expectation of survival, but you could hopefully improve the quality of the time they had left.
“Fast-forward to today. If you’re diagnosed with HIV as a 22-year-old and take medicine to control the virus, you can expect to live a near normal life span.”
That is a great leap forward in a relatively short time, but HIV still poses a threat around the world. In 2022, 39 million people were living with HIV and an estimated 630,000 died of AIDS-related illnesses, according to UNAIDS. And while there’s still no vaccine or cure, in just a few decades HIV has gone from a virtual death sentence for many to a manageable, chronic disease in the United States and most developed countries.
“I’m optimistic that we can end the epidemic in New York state in the next few years,” Dr. Merrick says.
NewYork-Presbyterian’s HIV clinics have provided care for 35 years, from the earliest days of the AIDS epidemic. And Drs. Gordon and Merrick were there almost from the start.
Dr. Gordon was a medical resident when he began treating patients at the Comprehensive Health Program, now comprising three HIV clinics: one for adults, another for teens, and a third for women, children, and young adults at NewYork-Presbyterian/Columbia University Irving Medical Center.
Dr. Merrick, meanwhile, finished his medical residency on a Friday in 1991 and began working that Monday at the Center for Special Studies, which has two adult HIV clinics: one at NewYork-Presbyterian/Weill Cornell Medical Center and the other in the Chelsea neighborhood of Manhattan.
Today, they serve as medical directors of these programs, and in commemoration of World AIDS Day on Dec. 1, Health Matters is sharing the reflections of Drs. Merrick and Gordon about the clinics’ legacy of HIV care — from the darkest days of the AIDS crisis to today’s intensified focus on ending the epidemic.

Dr. Samuel Merrick
Why were NewYork-Presbyterian’s HIV clinics created?
Dr. Merrick: Our clinic began in 1988 when new infection rates were exploding. New York City hospitals were filled with people with HIV. It was overwhelming them, and there was a fear that HIV would take over all the hospitals. It was staggering. Dr. Jonathan Jacobs, our founder who still sees patients here, felt this was a defining moment in medical history; that there was a great need. He wanted to design a system of care that could supply as many of the needs as possible in a multidisciplinary, comprehensive way. And we felt strongly that what patients needed was someone who knew them well. So we hired physicians who cared for them when they were hospitalized and when they were outpatients in the clinic — that continuity model.
Dr. Gordon: New York City was the epicenter of the epidemic in the United States, in terms of sheer numbers. A unique collaboration between AIDS activists and the state Department of Health led to the establishment of Designated AIDS Centers, which includes these clinics and later one at NewYork-Presbyterian Queens, that pioneered a comprehensive care delivery system for patients with HIV. This kind of integrated care, in which we cared for patients from inpatient, to outpatient clinics, and into the community, was visionary at the time. Our founders, Dr. Jay Dobkin and Dr. Karen Brudney, who continues to provide care in the clinics to this day, pioneered many of these approaches that proved to be successful.

Dr. Peter Gordon
What was groundbreaking about them?
Dr. Merrick: The clinics’ core services were primary care. But the greatest needs patients often had were not medical. So we had social workers, psychiatrists, nutritionists, a full-time chaplain for many years, and volunteer lawyers — mostly for planning for the children for when their parents died, healthcare proxies, and wills. We found that our patients wouldn’t go to other clinics for checkups, so we added things like a gynecologist, a dentist, and a dermatologist.
Dr. Gordon: Our clinic developed many services but never enough to meet the need as the epidemic swelled. Our co-located services included neurology and care for pregnant HIV-positive women as HIV was often passed, in the early years, from mother to child during pregnancy or labor. Also, many of our patients suffer from high rates of other challenging medical conditions, such as mental health and substance use disorders so we added those services. A perfect example is smoking, which is especially dangerous for people with HIV– yet the rate of smoking for people with HIV is twice that of the general population. So our clinic added tobacco cessation services.
What kind of stigma did people with HIV face in the early years?
Dr. Gordon: The stigma people experienced when they sought care elsewhere was profound, and patients were often turned away. If their HIV status was disclosed, they feared losing relationships, jobs, and housing. The stigma, along with the reality that there was no effective treatment, led many people to not want to know their HIV status even though they suspected they might be infected. Unfortunately, this fueled the epidemic as people unknowingly infected others. Though better now, stigma remains a problem to this day. I have very ill patients in the hospital right now who won’t take their HIV medicine because they don’t want people at home to know they have HIV.
Dr. Merrick: I remember in the early days being at a gathering where a guy I’d known in college asked me what I did. I said I was an HIV doctor, and he literally took a step back. And people would ask me questions like, “Well, I guess you expect to get HIV then don’t you?” There was a lot of fear even in the medical community. We had a lot of challenges getting people the medical care they needed. People would lose their jobs, their families. The overt discrimination was striking.
Drs. Gordon and Merrick recount the stigma against HIV/AIDS
What was it like for clinicians in the beginning?
Dr. Gordon: It was difficult as we knew that even patients with seemingly good health were likely to die in a relatively short period of time. A lot of the work was like hospice care. Everyone in the clinic was drawn to the work during this crisis because they truly cared and hoped that they could reduce the suffering.
Dr. Merrick: One week I had three patients die while I was physically in contact with them. But while 30 to 40 percent of our patients died every year, the rest didn’t — it depended on how badly damaged their immune system was at that time. I still have 15 or 20 patients who I started caring for when I first got here in 1991, including my very first appointment, because they were still alive when the new effective medicines finally came out.
Drs. Gordon and Merrick discuss being on the front lines of the HIV epidemic in the early days
What was the turning point for HIV?
Dr. Gordon: 1996 was a year that really changed things. It was a big year because modern antiretroviral therapy was born, which combined HIV drugs. We now had drugs that were effective, and the death rate for people living with HIV in New York City began to plummet. That was the moment when people realized that what had been a progressive, fatal disease in virtually every case could be transformed into a chronic illness with a good quality of life and a near-normal life expectancy.
Dr. Merrick: These combination therapies were truly miraculous. I had a patient who was admitted around that time with HIV dementia and “wasting,” or extreme weight loss, and he went to a skilled nursing facility to be in hospice care. And a year later, I saw his name on my schedule and then this guy walks in perfectly healthy. So it was that dramatic for people. Even people who were just hanging on by a thread, many of them were able to get their lives back.
How have these medications changed over the years?
Dr. Merrick: In the early days, the number of pills patients had to take could easily be north of 20 pills a day. For some, it could be 30 or 40 when you start adding in treatments for opportunistic infections. There was a lot of nausea, vomiting, diarrhea. They were toxic and difficult to take. It required scheduling to take three times a day on an empty stomach, which is incredibly challenging. So those early medications were not easy. Today, most people can take one pill a day. It’s a combination of usually three different medications. They’re quite safe.
Dr. Gordon: It’s miraculous that it’s now down in most cases to just one pill. The new medications are extraordinarily well-tolerated for most people, virtually no different than taking a medication for high blood pressure or diabetes.
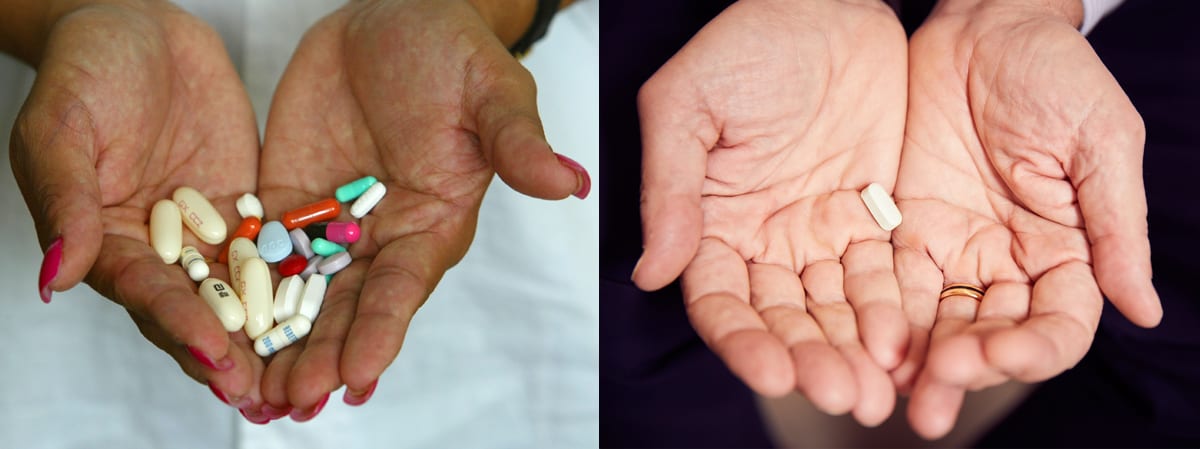
In the early days, patients often took 20 to 30 pills daily. Today, most people take one a day.
Were your HIV centers involved in treatment research?
Dr. Gordon: Both of our centers have always worked hand-in-hand with the research units of our affiliated medical schools and continue to do so today. Our patients volunteered in large numbers with the hope that they were getting access to effective medicine and to push the science forward. Our institutions, Columbia University Irving Medical Center and Weill Cornell Medicine, have been at the forefront of groundbreaking, scientific discoveries that have helped transform HIV care.
Dr. Merrick: The Weill Cornell clinical trials unit has been located right next to us from the beginning. And there really wasn’t another way to get a new medication other than enrolling in a trial and taking a chance. But there are also clinical trials for potential therapies that may not end up benefiting the patient. So very often, patients enroll out of a sense of altruism. They feel they’ve been helped and want to help others.
What is it like living with HIV today?
Dr. Gordon: For most people diagnosed today, they can expect to live a near normal life span if they take their medicine daily. While it’s a real medical issue they have to deal with, for many it may not even be their main medical challenge as they grow older, just a chronic condition that’s relatively easily dealt with.
Dr. Merrick: Also, the perception that you can’t have a normal relationship and have kids has changed. We know that when patients take their daily medicines and the HIV virus in their blood is undetectable, they can’t transmit the virus, so they can have healthy, loving relationships. And if one partner is HIV negative, he or she can take a preventive medication as added protection. Heterosexual partners with a negative and a positive partner can have condom-less sex and conceive naturally and safely.
How have things changed for babies and kids?
Dr. Merrick: We closed our pediatric clinic, thankfully, because there are virtually no new babies born with HIV in New York state. That’s because pregnant women with HIV now take medicine that prevents the transmission to their child. It’s a huge success. It was sad to say goodbye to our pediatric colleagues, but it was a very happy occasion to close the clinic.
Dr. Gordon: Today, teenagers and young adults are the groups at highest risk for new HIV infections. Our Project Stay program does outreach to at-risk teens on the streets, at schools, vocational training centers, centers for LGBTQ youth, community organizations, and through social media to promote sexual health and access to HIV preventive services. This is extremely vital work that is needed to move toward an AIDS-free generation, which is within our grasp.
Drs. Gordon and Merrick on caring for a generation of patients
Audio from 2018
What will it take to end the epidemic?
Dr. Merrick: NewYork-Presbyterian is playing a critical role in making the end of the HIV epidemic in New York City a reality. There are three pillars: We want to get people tested, we want to get people on therapy so their viral loads are undetectable, because “undetectable equals untransmittable,” and we want to do prevention. A big effort that we’re working closely together on is getting people on preventive medications known as PrEP and PEP to keep them HIV-free. PrEP is a daily pill or long-acting injection for people at high risk of acquiring HIV, and it vastly reduces their chance of getting it. For those who aren’t on PrEP, PEP is a pill to take after a high-risk exposure, like having sex with someone whose HIV status is positive or unknown. With all of these efforts, I’m very optimistic that we may be able to meet the state’s Ending the Epidemic goals in the next few years.
Dr. Gordon: In addition, NewYork-Presbyterian has launched significant new HIV prevention, testing and linkage-to-care services at several of our hospital campuses throughout New York City. We also plan to deploy a mobile medical unit to bring services and care right to NewYork-Presbyterian communities that experience high levels of new HIV infections. Another focus is our aging seniors with HIV, and we have new programs that promote physical exercise, socialization with peers and healthy lifestyles and wellness– much needed services for a community that has endured the unprecedented impact of the AIDS epidemic. This is all really promising and gives us confidence that with a final push, we really could see the end of HIV epidemic in New York in the next five years. We’re so close.
What drove you to do this work — all those years ago?
Dr. Gordon: Training in the early ’90s amid an HIV epidemic that was completely out of control had a powerful impact on me. I felt terrible at the plight of so many patients who I treated, and I deeply admired the people who founded and worked at the clinic and who committed their lives to making a difference. They were caring for people who desperately needed help, and that was something I wanted to be a part of. I’ve learned a lot about what is important in life through the courage, fortitude, and resilience of patients that we had the privilege of working with over the years.
Dr. Merrick: From the first day that I got here, what kept me going and still does is the people that I’ve been able to work with. They were so dedicated. It was hard to imagine doing anything else. I felt very fortunate to be in a place where, as difficult and challenging as it was, you felt like you were making a difference every day. And we get to work with a tremendous group of patients who are inspirational to us with their strength and resilience in the face of significant medical and life challenges. There was always hope in the back of your head that things are going to get better. And you wanted to be part of that and be there when it did get better.
Peter Gordon, M.D. is medical director of the Comprehensive Health Program, the HIV clinics at NewYork-Presbyterian/Columbia University Irving Medical Center. He also is professor of clinical medicine at Columbia University Vagelos College of Physicians and Surgeons.
Samuel Merrick, M.D. is medical director of the Center for Special Studies at NewYork-Presbyterian and Weill Cornell Medicine. He also is professor of clinical medicine at Weill Cornell Medicine.
Additional Resources
Both HIV centers are part of the NewYork-Presbyterian Ambulatory Care Network, which you can learn more about here.

