Patient With HIV Appears to Have Been Cured by Umbilical Cord Blood Transplant
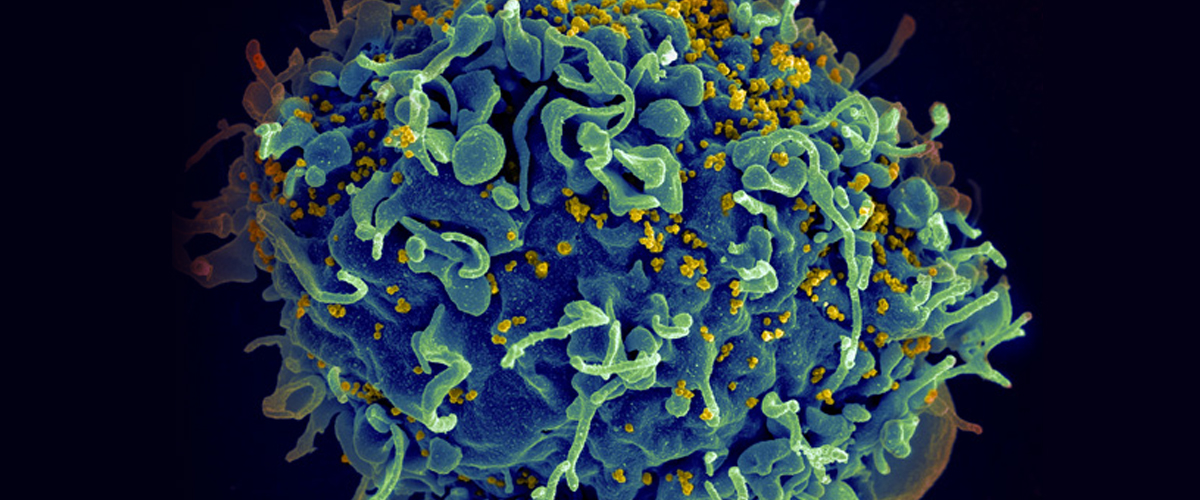
A human T cell (blue) under attack by HIV (yellow), the virus that causes AIDS.

A human T cell (blue) under attack by HIV (yellow), the virus that causes AIDS.
A patient appears to be the third person ever to be cured of HIV, following a transplant method involving umbilical cord blood. The patient’s doctors, a team of physician-scientists from Weill Cornell Medicine and NewYork-Presbyterian, presented details about the case at the 29th annual Conference on Retroviruses and Opportunistic Infections.
As part of leukemia treatment, the patient underwent a blood stem cell transplant, a medical procedure that replaces damaged immature blood cells with healthy ones. The transplanted cells came from umbilical cord blood from an unrelated newborn child, as well as from a healthy adult relative.
Cord blood is more widely available than adult stem cells and has a higher tolerance for a mismatch between the donor and recipient. The procedure’s apparent success in curing the patient’s HIV with cord blood opens up the possibility of curing a wider population of people with HIV who are in need of a transplant due to another condition such as leukemia. The cord blood donor cells bore a mutation that makes them resistant to HIV infection; the other two successful cases of an HIV cure involved the same mutation.
Three months after the transplant, tests showed that the patient’s blood cell population was entirely derived from the HIV-resistant cord blood cells, and HIV was no longer detected. The patient eventually stopped taking antiretroviral drugs to suppress HIV infection and has been off the HIV drugs for 14 months, with no signs of HIV reemergence after close follow-up. This indicates a likely cure, although physicians at this stage prefer to call it long-term remission. The patient has also been leukemia-free for more than four years.
Stem cell transplant specialists Dr. Jingmei Hsu and Dr. Koen Van Besien and infectious disease specialist Dr. Marshall Glesby were the physician-scientists who led the NIH-funded clinical trial at Weill Cornell Medicine in collaboration with investigators at University of California, Los Angeles; Johns Hopkins University School of Medicine; and several other institutions.
The investigators concluded that cord blood containing the mutation offers a possible cure for both hematological malignancies and HIV, and should be considered as a stem cell source when HIV-positive cancer patients need blood stem cell transplants. However, the procedure is considered too risky for HIV-positive patients who otherwise don’t need such transplants.
Many Weill Cornell Medicine physicians and scientists maintain relationships and collaborations with external organizations to foster scientific innovation and provide expert guidance. Weill Cornell Medicine and its faculty make this information available to the public to ensure transparency. External relationship information is available on the faculty profiles of Dr. Jingmei Hsu, Dr. Koen Van Besien, and Dr. Marshall Glesby.
— Adapted from Weill Cornell Medicine Newsroom

