In a GMA3 Interview, a Mom Meets the Altruistic Liver Donor Who Saved Her Son’s Life
What inspired a young paramedic from Massachusetts to become a living organ donor and save the life of a 2-year-old boy from North Carolina.
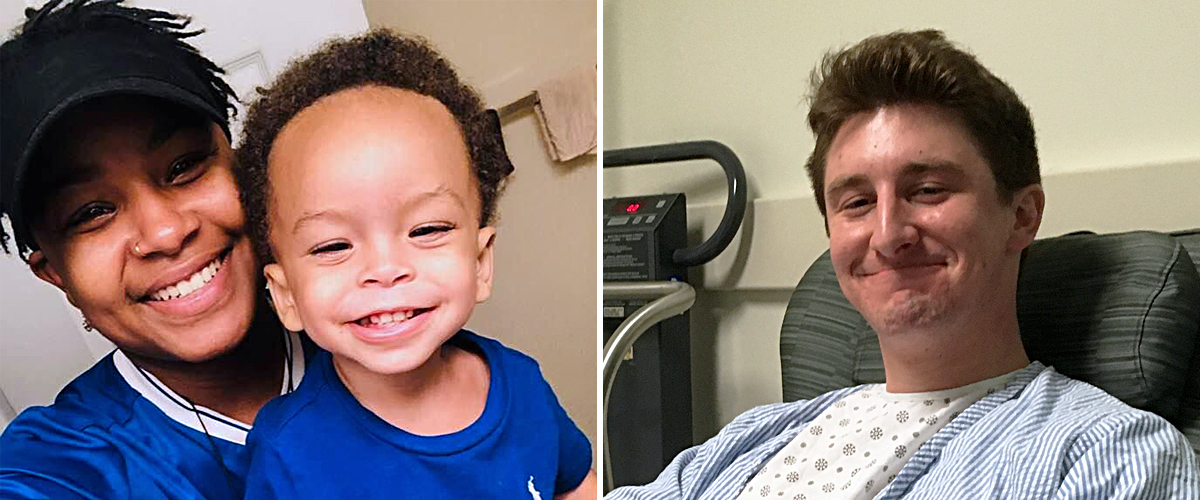

It was the moment Dia Landy had been thinking about for nine months. Suddenly she was face-to-face via Zoom with William Lindberg, the altruistic liver donor who saved her 3-year-old son, Ian Charles.
During a remote interview on GMA3: What You Need to Know, Dia was talking about how grateful she is for her son’s successful liver transplant at NewYork-Presbyterian in early February and how eager she was to meet the donor, when the hosts surprised the family by bringing Will on-screen so everyone could meet for the first time.
“I wasn’t expecting it!” says Dia. “We told Ian, ‘This is the guy! You have a piece of his liver in you. He saved your life.’ He smiled and said, ‘Oh, wow!’ Then he took off to grab some juice. He’s 3, he’s busy. He can’t sit still for long.”
But Will loved seeing Ian act like a typical toddler. “Ian is adorable, and it was a huge relief to see how well he was doing,” says Will. “He clearly is an active kid with a lot of energy.”
Just over a year ago, the circumstances were much different.

At age 2, Ian Charles was diagnosed with hepatoblastoma and needed a liver transplant.
While visiting family in New Jersey in September 2019, Ian’s dad, Paul Charles, noticed that a section of Ian’s belly felt hard while getting him ready for bed.
While Ian, then 2, didn’t complain of any pain or show any signs of a fever, “that night I couldn’t sleep very well,” says Dia. “Something told me, ‘Don’t brush this off.’”
Trusting her gut, Dia took Ian to the local emergency room in the morning. There, she says, “I got the worst news of my life.”
Doctors found a malignant tumor covering 75% of Ian’s liver and diagnosed him with hepatoblastoma, a rare type of liver cancer that can affect babies and young children.
Instead of returning home to Charlotte, North Carolina, doctors advised that Ian start chemotherapy immediately. Over five months and five rounds of treatment, Ian’s tumor decreased in size — but it was encasing a major artery, making it nearly impossible to surgically remove the mass.
By November 2019, Ian’s doctors delivered devastating news: Ian needed a liver transplant. The family was referred to NewYork-Presbyterian Morgan Stanley Children’s Hospital.
“It was a tough time. All of us were scared, not knowing what the outcome would be but trying to be strong for Ian,” says Dia. “I was terrified because I know a lot of people can be on transplant lists for months or years.”
More than 12,000 people in the U.S. are waiting for a liver transplant, according to the Organ Procurement and Transplantation Network. Instead of waiting for a deceased donor, Ian’s relatives quickly mobilized to see if any of them could be a match and become a living liver donor for Ian. But their search suddenly came to a halt.
“We learned Ian needed a transplant on a Monday,” recalls Dia. “About two weeks later, we learned there was a donor.”
“You Can Give Something … Without Truly Losing Anything”
Will was on duty as a paramedic around Cambridge, Massachusetts, when he responded to an emergency call from a patient with liver failure.
“When I was young, I lost my dad to pancreatic cancer, and I remembered that he was the exact same jaundice color as this patient,” says Will, who struck up a candid conversation with the patient during transport to the hospital. “The interaction pulled at my heartstrings and pushed my buttons in a couple different ways.”
After his shift, Will decided to read more about liver failure, which led him to learn a startling fact about liver transplants: The liver is the only organ that can regenerate, so an altruistic donor (also known as a nondirected donor) could donate part of their liver to a stranger, and the donor’s organ would grow back to its original size within six to eight weeks and function as normal.
Living liver donors, however, are not common. In 2019, there were 8,896 liver transplants performed in the U.S and only 524 of those took place thanks to a living liver donation, according to the United Network for Organ Sharing.
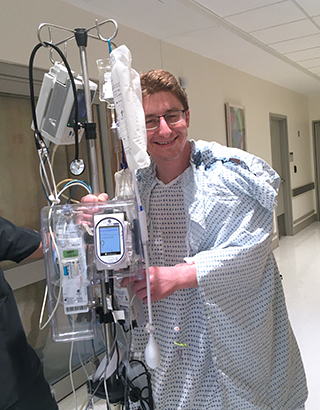
Will Lindberg post-transplant at NewYork-Presbyterian/Weill Cornell Medical Center.
“The idea that you have this ability to give something that’s so important without truly losing anything, that became wedged into my head,” Will says. “The more I read, it went from something that I could do to something I absolutely should do.”
Unfamiliar with the organ donation process, Will turned to the internet to find the best hospital for altruistic liver donors. Across all the online forums and community groups, NewYork-Presbyterian/Weill Cornell Medical Center kept popping up in his discussions with recipients and past donors. “That was really encouraging,” says Will.
At NewYork-Presbyterian/Weill Cornell Medical Center, Will learned that a portion of his liver would be removed through a minimally invasive laparoscopic procedure that involves a 3-inch incision above the pubic bone. Typically, recovery time in the hospital ranges from four to six days, depending on if the organ donor is matched to a child or an adult. Post-transplant, organ donors can expect to feel normal within four to six weeks.
“Every point along the way, people would present the next few hurdles that I would have to face, and each time it didn’t sound that bad,” says Will. “The whole process didn’t sound insurmountable.”
“Will is a very generous person,” says Dr. Benjamin Samstein, chief of liver transplantation at NewYork-Presbyterian/Weill Cornell Medical Center and Will’s surgeon. “He’s also a man of action. He likes to do things rather than just talk about them.”
While Will always imagined that he would donate to an older recipient like his father, he was shocked to find out he was matched with a young boy with liver cancer.
“I had spent a lot of time wondering what my recipient and his family were going through while moving through the donation process,” recalls Will. “In particular, I remember thinking the night before our surgeries how his parents must be facing such of a mix of hope and fear.”
When Dia heard that an anonymous 28-year-old man had stepped up to donate his liver just because, she was speechless. “He’s so young and that was very selfless of him to do,” she says. “That says a whole lot about his character. We love him for giving up a part of himself to save someone — and a child at that.”
The Gift of Life
The morning of February 4, 2020, Ian and Will prepared for surgery across town from each other — Ian at NewYork-Presbyterian Morgan Stanley Children’s Hospital and Will at NewYork-Presbyterian/Weill Cornell Medical Center.
Dr. Samstein removed about 20% of Will’s liver, which was then rushed via an organ transport ambulance to the operating room by Dr. Adam Griesemer, a transplant surgeon at the Center for Liver Disease and Transplantation at NewYork-Presbyterian. There Dr. Tomoaki Kato, chief of the Division of Abdominal Organ Transplantation at NewYork-Presbyterian/Columbia University Irving Medical Center, was preparing Ian to receive the liver. Together, Dr. Kato and Dr. Griesemer removed the toddler’s liver and implanted the portion of Will’s liver in a six-hour procedure.
“Living donor liver transplantation is a life-saving procedure. Because the size of the liver necessary for children is relatively small, it is particularly valuable for children like Ian,” says Dr. Kato. “The procedure is technically demanding because it requires surgical precision and careful coordination of the team. We are one of the most experienced centers for it.”
“We love Will for giving up a part of himself to save someone.”— Dia Landy
Following the complex procedure, “Ian was so resilient,” his mother says. After surgery “he woke up still hooked up to machines and he tried to stand up to get out of the crib. He was pulling up, trying to walk.”
Ian made his way through his 10-day recovery against the backdrop of a looming COVID-19 pandemic that never interrupted the care he received at NewYork-Presbyterian Morgan Stanley Children’s Hospital. Even as worries mounted over the coronavirus, “I loved the way that they cared for my son and all the other patients coming in and out of the hospital,” Dia says of Ian’s multidisciplinary team. “The passion they have for children there is unmatched.”
One month after the transplant, Ian completed his final round of chemo and has been cancer-free since. Ian will need follow-up care throughout his life, but his new liver will grow and meet Ian’s evolving needs, explains Dr. Jennifer Vittorio, a transplant hepatologist at NewYork-Presbyterian Morgan Stanley Children’s Hospital and a member of Ian’s care team.
“He is high energy and much more interactive,” says Dr. Vittorio, who is also an assistant professor of pediatrics at Columbia University Vagelos College of Physicians and Surgeons.
“The whole time, he kept a smile on his face. He never stopped running around or playing, even if he didn’t feel very well. He didn’t skip a beat,” Dia says of Ian. Nowadays “he’s definitely back to himself. He’ll even point to the scar on his stomach and say, ‘Mom, look!’”
As for Will, despite a rare post-transplant complication and a bout of the flu after surgery, he rebounded within a month and returned to work in Cambridge, where he periodically follows up with his transplant team via telehealth visits.
Ian Turns 3!
After overcoming a year of great uncertainty, the family was thrilled to celebrate Ian’s third birthday August 3 thanks to the gift of a lifetime from Will.

Now cancer-free, Ian Charles celebrated his birthday on August 3, 2020.
“This highlights how altruistic donation allows us as a community to assist each other in times of need,” says Dr. Vittorio.
Dia and Ian were cleared to return home to North Carolina in September — one year after Ian’s initial diagnosis — where Dia says Ian looks for any excuse to play outside, wrestles with his cousins, and continues to thrive.
“There’s nothing I can say or do for Will to show all my gratitude for saving my son’s life,” Dia says. “He gave us our baby back.”
Says Will, “I just hope that Ian can enjoy being a kid, without the extra stress involved with being really sick and having to spend so much time inside a hospital.”
Dia and Will continue to text each other, and Dia is already planning for the moment when Will can safely visit the family’s North Carolina home.
“I invited him to a cookout once COVID is over,” says Dia. “A cookout with the Landy family is all about soul food, music, and family — and Will is family now.”
To learn more about becoming a living organ donor, visit nyp.org/organdonor.

