A New Heart for Baby Ruby
Born with a rare and potentially fatal heart disease, Ruby Cotter underwent a transplant at 6 months old and proved “nothing will bring her down.”
When Ruby Cotter turned 10 weeks old, she was fussier than usual. Her parents, Ashley and Brian, thought it could have been for any number of reasons: Ruby started a new supplemental formula. She didn’t eat much during her usual 3 a.m. feeding. And the day before, Ruby had spit up in a more animated way, so maybe she was coming down with a bug.
But as the morning progressed on September 4, 2019, Ruby took a turn for the worse. “Her limbs were cold, but her core was warm, and she was just so tired,” says Ashley. After a meager morning feeding, Ruby started dry heaving. When Brian and Ashley checked Ruby’s temperature, the thermometer read 96 degrees.
“My gut said something is not right,” says Ashley. “I called our pediatrician, who said, ‘Don’t waste your time coming into the office; go straight to the ER.’”
Ashley and Brian rushed Ruby to a hospital and “within 10 minutes of our arrival, Ruby was not breathing,” Ashley says. “They took her into a room and had to intubate her. When we saw her later in the pediatric intensive care unit, they had stabilized her, but she had wires and tubes coming out of her. It was heartbreaking.”
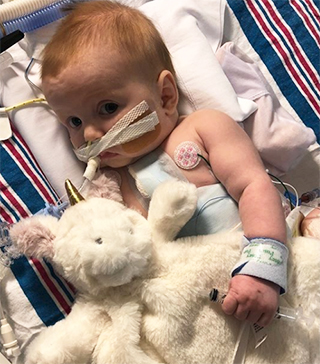
At 3 months, Ruby Cotter was placed on the transplant list for a new heart.
An echocardiogram revealed that Ruby suffered from heart failure due to dilated cardiomyopathy, a condition in which the left ventricle of the heart stretches and becomes thinner. As a result, the enlarged heart struggles to contract and pump blood through the body. The rare heart disease, which is thought to be caused by a genetic predisposition or a viral infection, affects about 4 in 100,000 infants under 12 months.
“The ER doctor said if we hadn’t brought her in when we did, she would not have made it,” says Ashley.
The doctors were also certain about where Ruby needed to go for further treatment: That same day, she was transported to NewYork-Presbyterian Morgan Stanley Children’s Hospital.
The team there, which included Dr. Irene Lytrivi, pediatric cardiologist in the Program for Pediatric Cardiomyopathy, Heart Failure, and Transplantation at NewYork-Presbyterian Morgan Stanley Children’s Hospital, immediately put Ruby on IV medications in an attempt to take some of the stress off her heart and to see if her body would heal and recover with medication.
But after a week, when they tried to wean Ruby off support for breathing and eating, “her heart rate jumped up to 300 beats per minute,” says Ashley.
When it was clear that Ruby’s heart couldn’t support her and medications weren’t effective, “they put her on the list for a transplant,” says Ashley.

Dr. Irene Lytrivi
A Temporary Lifeline
The wait for a pediatric heart transplant can be three to nine months. During that time, Ruby could have remained sedated and intubated until a donor heart came through.
The other option was for Ruby to undergo surgery to implant a Berlin Heart, a ventricular assist device (VAD) that is a small, external pump that does the work of the heart and maintains blood flow in babies with severe heart failure. The device is a temporary solution that would allow Ruby to thrive and live as normal of a life as possible while waiting for a new heart.
“The team thought the assist device would be the best option, and the family decided to go for it,” says Dr. Lytrivi, who is also an associate professor of pediatrics at Columbia University Vagelos College of Physicians and Surgeons.
On September 12, Dr. David Kalfa, a pediatric and congenital cardiac surgeon at NewYork-Presbyterian and assistant professor of surgery and surgical director of the Initiative for Pediatric Cardiac Innovation at Columbia University Vagelos College of Physicians and Surgeons, performed open heart surgery to insert the Berlin Heart. “The surgery went extremely well,” says Dr. Kalfa. “She responded very well to the implantation of the VAD.”
“Ruby was the poster child for an assist device,” adds Dr. Lytrivi. “She didn’t have any neurologic events. There wasn’t any significant bleeding. She was extubated quickly. She did everything that we hope kids with assist devices will do.”
Well, almost. As Ruby gained back some of her strength in the weeks after her surgery, “she would play and lift her Berlin Heart with her feet and give me a heart attack,” says Ashley.
“It didn’t bother Ruby that she was in the hospital or that she was hooked up to a machine,” adds Ashley. “The nurses loved that about her because it means she is resilient, and nothing will bring her down.”
Waiting for a Heart
Following the Berlin Heart surgery, the real waiting game began. Ashley and Brian moved into Ruby’s room in the intensive care unit at NewYork-Presbyterian Morgan Stanley Children’s Hospital to help their daughter recover and remain strong for when a heart became available.

After her first open heart surgery, Ruby learns to feed from a bottle again with her mom’s help.
Over the next three months, the couple were actively involved with Ruby’s physical therapy to teach her how to hold her head up and feed from a bottle again. They took Ruby for wagon rides around the unit. Brian’s silly faces elicited Ruby’s first giggles while she was in her hospital bed. And they learned how to give Ruby baths and change the dressings around her Berlin Heart.
“What I love about the hospital is that they include you. They want you to be a part of what’s happening with your child,” says Ashley. “During the morning rounds, they come and explain everything to you. And if you don’t understand something, you can ask them 20 million questions, and they’ll talk to you about all of them.”
Ruby, however, did play favorites among the hospital staff. “We have a special place in our hearts for Dr. Lytrivi,” says Ashley. “She and Ruby have a very special connection. Whenever Ruby sees her, she always lights up and smiles.”
Despite all the incredible progress, there were lots of emotional highs and lows. After more than three months of waiting for a heart transplant, “I was thinking, ‘We’re going to be here forever. A heart is not going to be available,’” acknowledges Ashley. “I was losing hope even though Ruby was doing so well.”
On December 21, as Ashley and Brian were watching an episode of Master Chef in Ruby’s room, Dr. Lytrivi appeared at the door with the news they had been hoping for. “She said, ‘We have a heart and we think it’s a good match,’” recalls Ashley. “I was in a state of shock.”
“I get emotional every time I say it,” says Dr. Lytrivi, who explained to the Cotters that while the donor heart was a possible match on paper, the hospital’s procurement team still had to examine and harvest the organ. If everything worked out, Ruby would get a new heart the next day.
“It’s an amazing moment,” says Dr. Lytrivi. “But at the same time, there is the agony about going back to the ER, especially for kids like Ruby who have already gone through this once.”

Dr. David Kalfa
The Cotters weren’t worried. “They were prepping Ruby the night before the surgery, and I didn’t feel scared,” says Ashley. “It was emotional, but I trusted the process, which speaks a lot to the doctors and nurses. If I didn’t trust them, I probably wouldn’t have felt like that.”
On December 22, Dr. Kalfa opened Ruby’s chest once more, this time to remove the Berlin Heart and successfully transplant a new heart in an eight-hour procedure. Ruby’s surgery was one of 30 pediatric heart transplants that were performed on children under 18 at NewYork-Presbyterian Morgan Stanley Children’s Hospital in 2019.
“The surgery went extremely well. There were no issues, no complications, no bleeding. The function of the heart was excellent right after the surgery,” says Dr. Kalfa. “It’s so rewarding to see a baby get a new heart. It’s a fantastic feeling.”
“Ruby is our hero in every way,” Ashley said after the transplant. Since she was admitted to the hospital in September, “she has gone through four months of fighting and overcoming. She is powerful and strong because of this beautiful gift of life. And because of all the wonderful nurses and doctors, she has a chance at a normal life.”
Returning Home
Following the transplant, “I feel like Ruby has exceeded everyone’s expectations,” says Ashley.
The Cotters finally returned home as a family on January 7, just over two weeks after Ruby received her heart. She has had monthly biopsies to monitor for any signs of the body rejecting the new heart as well as regular blood work.
“Every time we touch base with the team, and they see her, they’re just thrilled with all the milestones she’s able to hit,” says Ashley. “I don’t know if we could have asked for a better outcome from her transplant.”
“Ruby is our hero in every way… And because of all the wonderful nurses and doctors, she has a chance at a normal life.”— Ashley Cotter
Since the COVID-19 pandemic hit New York City in March, Ruby has shifted to a mix of telehealth and in-person visits.
“We try to do 50% of each patient’s visit via telehealth and 50% in person,” says Dr. Lytrivi. After surgery, even before the outbreak, “we asked Ruby’s parents to be a little more careful with handwashing and to socially distance from sick contacts. In many ways, the way they lived pre-COVID is how the rest of us are learning to live now.”
Throughout the outbreak, Ashley and Brian still drove Ruby to NewYork-Presbyterian Morgan Stanley Children’s Hospital for monthly blood work because “they know her there,” says Ashley.
The hospital also provides transplant families with a hotline number. “We’ve called when we’ve had instances where she’s thrown up her medicine or we needed a prescription refill,” says Ashley. “We have the doctors’ emails. We can always reach out to them. They’re always in communication with us on lab results. The team is phenomenal. They have been there for us 24/7.”

Ashley and Brian Cotter at home with their daughter Ruby post-transplant.
Ruby Turns 1!
When Ruby turned 1 on June 12, she was a very different baby compared to nine months ago.
“She is starting to try to stand,” says Ashley. “She actually throws herself off the couch. She’s a lunatic!”
Ruby will soon have to make room for another bouncing baby on the couch: Ashley and Brian are expecting their second child this winter. “I am a little bit nervous because we did the genetic testing and nothing was really conclusive as to why this happened to Ruby,” says Ashley.
She is certain Ruby will adjust to being a big sister. “I think she’s going to do great. She’s tough,” says Ashley. “This kid lives life on the edge.”
And life after transplant doesn’t mean Ruby has to slow down anytime soon, even though she has to take immunosuppressants for the rest of her life to prevent her body from rejecting the heart and will likely need another transplant when she’s much older.
Overall “she can have a normal quality of life,” says Dr. Lytrivi, “and we expect advances in medicine will have her living a long time.”
Ashley and Brian are grateful to the team at NewYork-Presbyterian Morgan Stanley Children’s Hospital for making that a reality. “All of them cared so much for Ruby,” says Ashley. “They really saved her.”

