Birth Control Options: Choosing the Right Type
From pills to patches to IUDS, an OB-GYN explains how the various types of contraceptives differ.
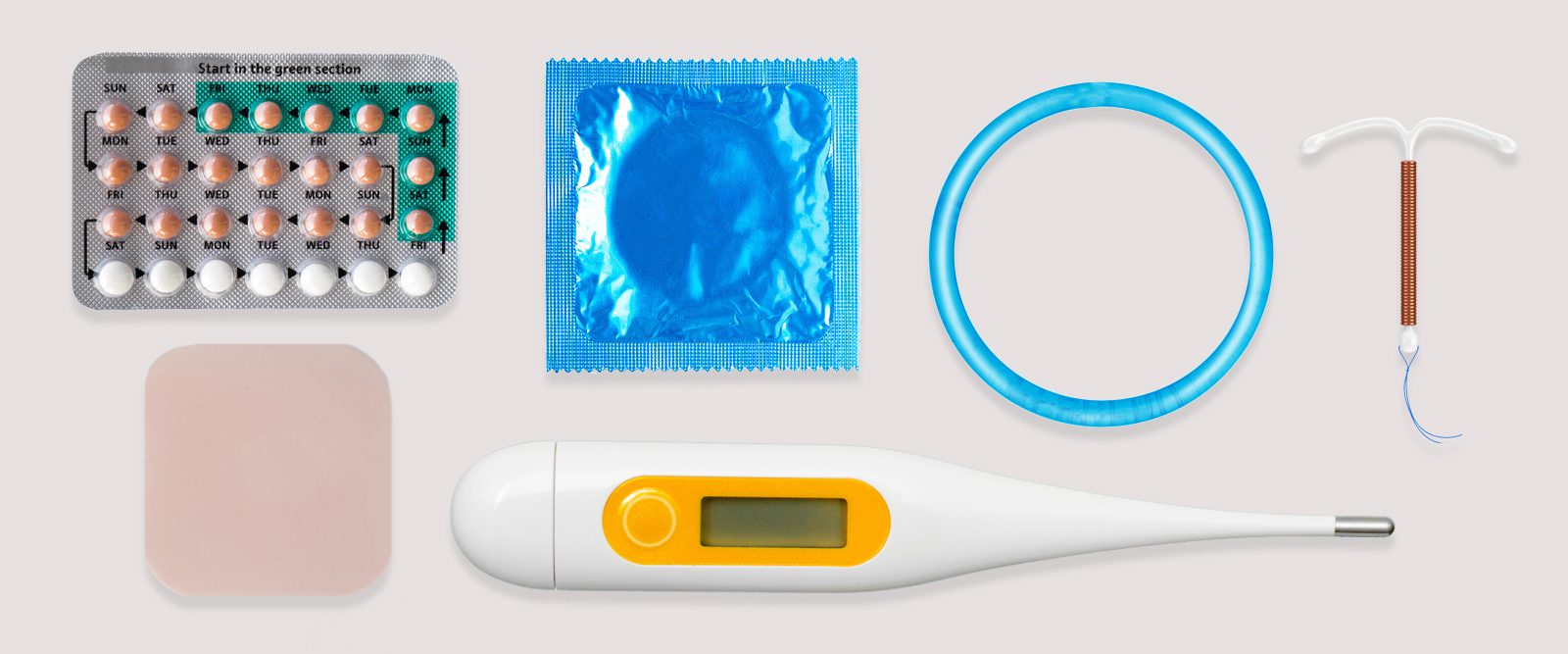
Taking control of your reproductive health is essential when planning your family and making decisions about how to prevent pregnancy. But, with a variety of birth control options available today, it can be overwhelming to figure out which method is right for you.
“When choosing a birth control, knowing its effectiveness is key,” says Dr. Aileen Gariepy, obstetrician and gynecologist at NewYork-Presbyterian/Weill Cornell Medical Center and the director of Complex Family Planning at Weill Cornell Medicine. “It’s also important to consider things like how often you have sex, future pregnancy plans, your ability to use certain methods as prescribed, side effects, any health conditions you may have, convenience, and protection against sexually transmitted infections (STIs).”
Health Matters spoke with Dr. Gariepy, who discusses the different types of birth control options — from most effective to least effective, based on typical use — and how each works.

Dr. Aileen Gariepy
Most effective methods
Most effective methods
Permanent birth control
Effectiveness: Nearly 100% effective
How they work: These methods permanently prevent pregnancy. They are intended for individuals or couples who have decided that they don’t wish to have children or have completed childbearing.
Examples:
- Tubal ligation or removal: Tubal ligation, also known as “getting your tubes tied,” or sterilization, is a surgical procedure for women. It involves removing or blocking the fallopian tubes to prevent the sperm and egg from combining.
- Vasectomy: Vasectomy is a surgical procedure for men. It involves cutting or blocking the vas deferens, the tubes that carry sperm, preventing sperm from mixing with semen.
Other things to know: While it’s possible that some surgical techniques for sterilization can be reversed in some cases, the success of reversal varies, and it is not guaranteed. Those considering permanent contraceptive methods should be certain of their decision and discuss all options with their doctor.
Long-acting reversible contraceptive (LARC) methods
Effectiveness: 99% effective
How they work: LARC methods work by providing highly effective long-term contraception. “These are ‘set it and forget it’ methods, and are really effective for people who know they do not want to get pregnant for a few years,” says Dr. Gariepy. A healthcare provider inserts one of the devices in the office.
Examples:
- Contraceptive arm implant: A small, matchstick-sized rod inserted under the skin of the upper arm that releases hormones to prevent pregnancy. It is FDA-approved for up to three years but effective for up to five years. The implant can be removed at any time if someone no longer wants it or wishes to get pregnant.
- Hormonal intrauterine device (IUD): A small T-shaped device inserted into the uterus that releases progestin, thickening cervical mucus and blocking sperm. Lasts from three to eight years, depending on the IUD brand.
- Copper IUD: A small T-shaped device inserted into the uterus. Unlike hormonal IUDs, they release copper, which is toxic to sperm and prevents fertilization (joining of the egg and sperm). Lasts up to 10 years.
Other things to know: “The availability, safety, and effectiveness of these LARC methods to decrease unintended pregnancy have been one of the major public health gains over the last few decades,” says Dr. Gariepy. Once removed, fertility typically returns promptly, allowing you to plan for pregnancy when ready.
Effective methods
Effective methods
Hormonal methods (Short-acting)
Effectiveness: 90% effective, on average
How they work: These methods release hormones into the body to prevent ovulation (egg release from the ovary) and thicken cervical mucus, which prevents the sperm and egg from joining.
Examples:
- Birth control shot (Depo-Provera): This is an injection contraceptive that releases progestin into the body to prevent ovulation. A healthcare professional administers it every three months.
- Combined oral contraceptives (“the pill”): Pills containing the hormones estrogen and progestin, which prevent ovulation. These pills should be taken at the same time every day. There are many different types, with varying hormone levels to suit individual needs. They are safe to take long term.
- Progestin-only pills: Daily oral pills that contain only progestin. They also need to be taken at the same time every day and have even less room for error than combined oral contraceptives. These “mini pills” will soon be available over-the-counter without a prescription.
- Contraceptive patch: A small patch applied to the skin that releases estrogen and progestin. It is changed weekly, with one week off per month to have a menstrual period.
- Vaginal ring: A flexible ring inserted into the vagina where it releases hormones (estrogen and progestin) to prevent ovulation. After three weeks, it is removed, and a new ring is inserted after a one-week break, if desired, to allow for menstruation.
Other things to know: For the pill, “An effective strategy for taking it at the same time every day is to partner it with something you’re already doing, like brushing your teeth,” says Dr. Gariepy. “Setting an alarm on your phone also helps.” Hormonal birth control can also be used to help with things like acne, irregular periods, and symptoms of PMS, endometriosis, and polycystic ovary syndrome (PCOS).
Less effective methods
Barrier methods
Effectiveness: 80% effective, on average
How they work: Barrier methods create a physical barrier between the sperm and the egg. This prevents fertilization and therefore prevents pregnancy.
Examples:
- Diaphragm: A shallow, dome-shaped device inserted into the vagina to cover the cervix and prevent sperm from reaching the uterus. It should be used with spermicide, which kills sperm, to work most effectively.
- Condom: Prevents sperm from entering the uterus by covering the penis or lining the vagina. Condoms are available for both men and women. They also provide the best protection against STIs.
- Cervical cap: Similar to a diaphragm, it is a smaller dome that fits over the cervix to block sperm and should be used with spermicide for better protection.
- Sponge: A soft, squishy device that is coated with spermicide. Inserted into the vagina before sex, it creates a barrier at the cervix, blocking sperm from entering the uterus. Keep in mind, though, it is less effective for women who have already had a baby.
Other things to know: Barrier methods must be used every time a person has sex. “Their effectiveness is so reliant on humans using them correctly,” says Dr. Gariepy. “For example, for condoms to be effective, you have to have one available that’s not expired, put it on before there’s any contact, leave room at the tip so there’s room for the ejaculate, and take it off right after the male ejaculates. That’s a lot for someone to get right, and we know that sex is not always planned.” For optimal protection and to prevent STIs, the condom can be used with another type of birth control.
Least effective methods
Natural family planning
Effectiveness: 76% effective
How it works: Also called fertility awareness, this option means tracking fertility signs so you can avoid sex or use another type of contraception during fertile days to prevent pregnancy.
Examples:
- Calendar method: This method involves tracking your menstrual cycle so you’ll know when your ovaries release an egg each month. It works best if you have regular periods.
- Basal body temperature method: By taking your basal body temperature every morning before you get out of bed, you can identify ovulation.
- Cervical mucus method: Monitoring changes in cervical secretions (cervical mucus) helps identify fertile days.
Other things to know: It’s most effective to use all three methods together. “This method requires that you take the time to check and chart your fertility signs every day,” Dr. Gariepy says. “It’s important to have a clinician teach you how to do this correctly.”
Overall, Dr. Gariepy notes, it’s important to remember that any method of birth control is more effective than no method. She adds, “For people who are having sex regularly over the course of a year and are not using a form of birth control method, their chance of pregnancy is about 80%.”
Aileen Gariepy, M.D., M.P.H., M.H.S., is a board-certified obstetrician and gynecologist at NewYork-Presbyterian/Weill Cornell Medical Center and an associate professor of obstetrics and gynecology at Weill Cornell Medicine. Dr. Gariepy is a fellowship trained sub-specialist in Complex Family Planning. Dr. Gariepy is a fellow of the American College of Obstetrics and Gynecology and serves on the Society of Family Planning’s Board of Directors and the American Medical Women’s Association’s Reproductive Health Coalition Steering Committee.
