RSV Cases on the Rise: What to Know
A pediatric pulmonologist shares insight into the respiratory virus that has seen a national spike in cases.

Cases of respiratory syncytial virus infection (RSV) — a common respiratory virus that causes mild, cold-like symptoms but can be severe for infants and older adults — are on the rise in the United States. From October 15 to 22, there were a total of 7,334 positive RSV results, according to the Centers for Disease Control and Prevention (CDC), which tracks detections of the virus every week. That number was at 1,241 in mid-August and positive cases have continued to mount since.

Dr. Hossein Sadeghi
Dr. Hossein Sadeghi, a pediatric pulmonologist and director of the Sue and John L. Weinberg Cystic Fibrosis Center at NewYork-Presbyterian Morgan Stanley Children’s Hospital, said that the rise could be due to the loosening of COVID-19 mitigation efforts, such as masking, social distancing, and limitations on travel. “Most children, by the time they were two years of age, had at least one episode of RSV infection, which helped them build immunity,” says Dr. Sadeghi, who is also an associate professor of pediatrics at Columbia University Vagelos College of Physicians and Surgeons. “That changed with pandemic precautions and isolations in the past few years.”
With flu already on the rise and concerns for another wave of COVID-19 cases, experts are concerned that the spike in RSV could signal a “tripledemic” this winter. According to the CDC, RSV causes 58,000 hospitalizations and 100 to 300 deaths among children under 5 each year. In adults 65 and older, an estimated 177,000 are infected with RSV, resulting in 14,000 deaths annually.
Dr. Sadeghi spoke with Health Matters to help understand the signs and symptoms of RSV, how to protect your family from the virus, and when to seek medical attention.
Who does RSV affect? Who is most vulnerable?
Dr. Sadeghi: RSV can affect anyone, typically presenting like a cold and usually clearing up with plenty of rest and fluids, but those who are most at risk for developing severe symptoms are premature infants or people with underlying conditions or a weakened immune system. For example, babies who are born after less than 29 weeks of gestation, people who are 65 years or older, and anyone with chronic lung disease, congenital heart disease, or neuromuscular conditions, may experience RSV symptoms more severely.
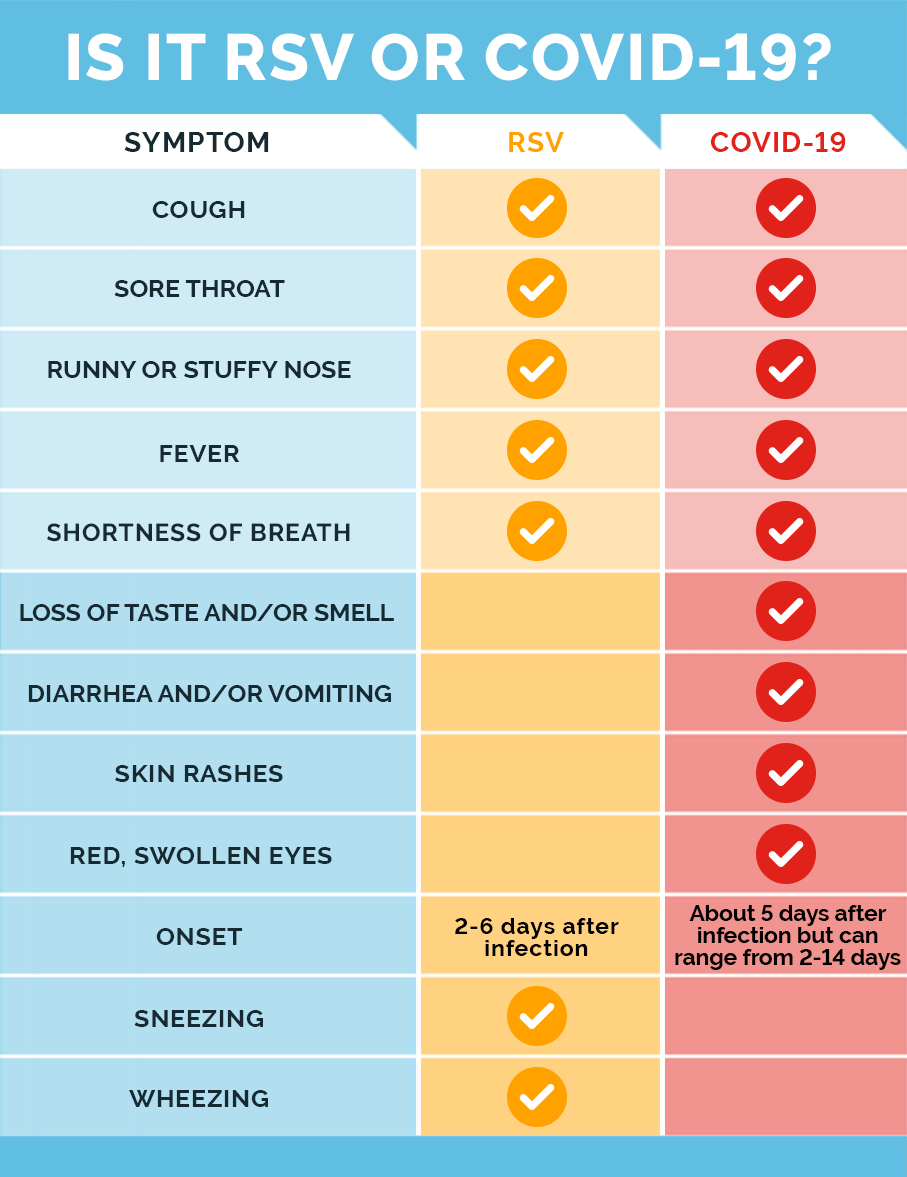
What are the signs and symptoms?
They typically include a runny nose, coughing, sneezing, wheezing, fever, and a decrease in appetite. Symptoms can appear within four to six days and last for seven to 10 days.
A sign of RSV in babies, which may be more serious since their immune system is still developing, is when they appear to be having a harder time breathing, such as wheezing, nasal flaring, or belly breathing. Belly breathing is when their ribs are visibly going in and out. Another clue is when they are feeding less, meaning their milk or food intake has reduced compared to before.
Why is RSV dangerous for infants?
RSV is more dangerous in babies because their immune system is still developing. In babies, RSV can cause bronchiolitis (inflammation in the small airways of the lungs), pneumonia, or croup, which can lead to breathing difficulties and a persistent cough. For premature babies, they could end up in the intensive care unit.
What are your recommendations for parents? How can they tell the difference between RSV and other viruses, like COVID-19?
Caregivers should be vigilant about infection control, know the signs and symptoms, and when to seek medical attention — the sooner the better. It is hard to distinguish one virus from another, so it is best for parents to contact their child’s pediatrician if the child is displaying signs and symptoms of RSV that continue with little to no improvement.
What are some tips to prevent transmission?
Taking preventive measures is crucial, especially for those who are at higher risk like premature babies or children with other risk factors. RSV can stay on hard surfaces for up to six hours, so handwashing and regularly disinfecting high-touch surfaces like doorknobs, countertops, and sinks are very important.
If there is an older child in the family who goes to school or daycare, I recommend changing their clothes as soon as they get home, washing their hands, and maybe even giving them a bath to reduce the risk of RSV transmission to a younger sibling.
Avoid close contact with anyone who is sick, and, of course, for any infection that we have vaccinations for — like the flu and COVID-19 — it’s important to immunize those who are eligible. The best defense against COVID-19 and the flu is to get vaccinated for both.
Are there medications to relieve symptoms? How can RSV be treated at home?
There is a medication called palivizumab (Synagis), a monoclonal antibody — an immune system protein — which works for infants who have chronic lung disease, are born prematurely, or if they have congenital heart disease. They can be immunized on a monthly basis so that when they get an RSV infection, they can handle it better. There are reduced rates of intensive care unit admissions or hospitalizations with this medication, but taking it does not mean that they are not going to get it. They can still get it. But the whole idea is that it is less severe.
RSV can be treated at home by getting plenty of rest and fluids. There currently is no vaccine for RSV, but most infections will go away on their own within a week or two. Parents can help relieve fevers with an over-the-counter fever reducer and pain relievers like acetaminophen or ibuprofen. For high-risk infants, parents should talk with their pediatrician about palivizumab, which can be given to them every 28 to 35 days during the RSV season.
Hossein Sadeghi, M.D., is a board-certified pediatric pulmonologist and sleep medicine specialist with extensive experience in cystic fibrosis, asthma, and global health. He is the director of the Sue and John L. Weinberg Cystic Fibrosis Center at NewYork-Presbyterian Morgan Stanley Children’s Hospital. An associate professor of pediatrics at Columbia University Vagelos College of Physicians and Surgeons, he focuses his research on asthma, RSV bronchiolitis, and cystic fibrosis.