Blood Donation: Who Can Donate Under the New FDA Guidelines?
The FDA updated its blood donation policy to broaden donor eligibility, making it more inclusive and potentially boosting donations.
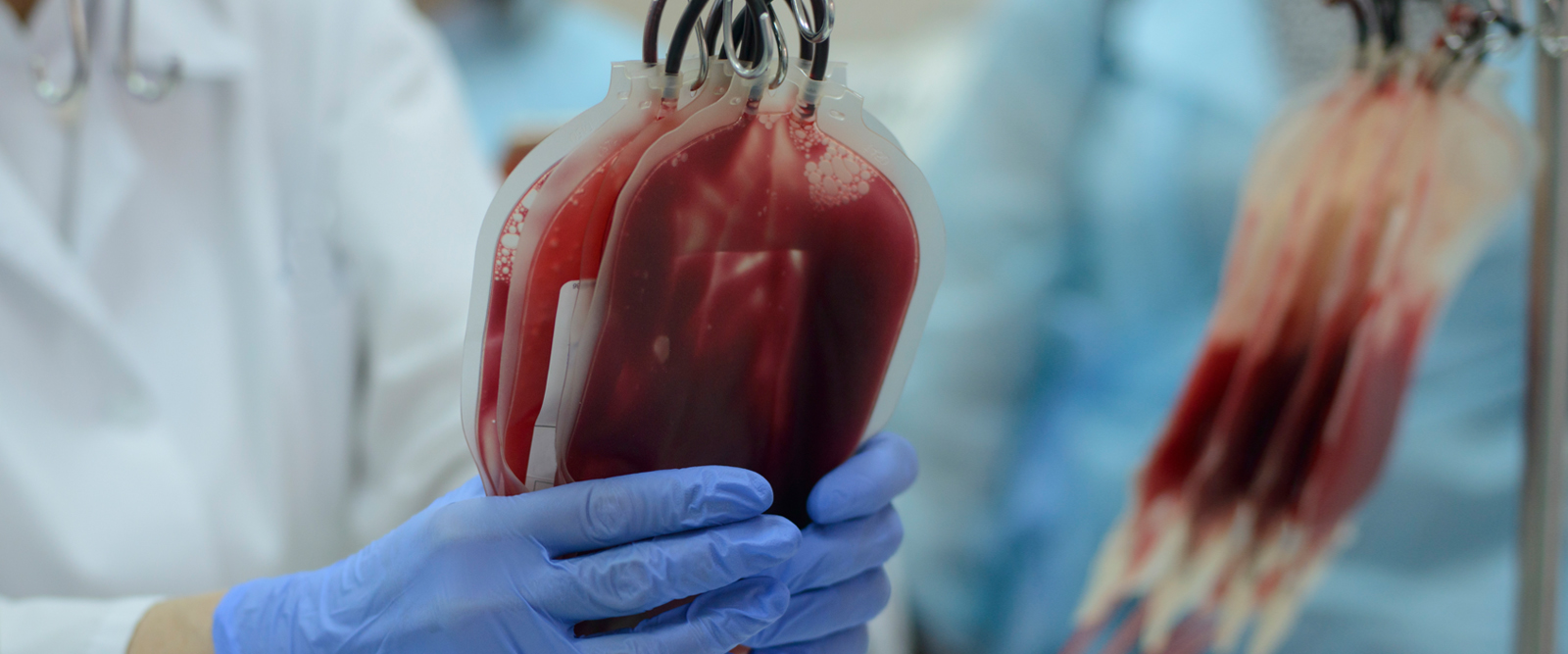

The Food and Drug Administration (FDA) recently announced a change to blood donation guidelines which will allow more gay and bisexual men to donate, doing away with decades-old restrictions.
Under the new recommendations, blood donor eligibility will not be based on sexual orientation, but rather individual risk-based questions. The questions, which are designed to reduce the risk of transfusion-transmitted HIV, will be the same for every donor, regardless of sexual orientation, sex, or gender, according to the FDA.
“There were many people who previously were not allowed to donate, and now they can,” says Dr. Sarah Vossoughi, the medical director of apheresis and associate director of transfusion medicine and cellular therapy at NewYork-Presbyterian/Columbia University Irving Medical Center. “We need everybody who can donate. I think this change will be good for the country to help diversify and increase our blood supply.”

Dr. Sarah Vossoughi
In 1985, the FDA had implemented a ban on blood donations from gay and bisexual men, in part due to limited testing. That ban remained in effect until 2015, when guidelines changed to allow men who had sex with men to donate if they abstained from sex for one year. A 2020 FDA update changed the deferral period to three months.
Now, with the universal implementation of risk-based questions, even more gay and bisexual men will be eligible to donate blood. Blood centers across the country will likely be able to implement these changes as early as the fall of 2023.
New FDA Guidance for Blood Donation
- No time-based deferrals for men who have sex with men (MSM) and women who have sex with MSM.
- All prospective blood donors will answer a series of individual, risk-based questions to determine eligibility.
- All prospective donors who report the following will be deferred to reduce the likelihood of donations by individuals with new or recent HIV infection:
- Having a new sexual partner, or more than one sexual partner in the past three months and having anal sex in the past three months.
- Taking medications to treat or prevent HIV infection, such as antiretroviral therapy (ART), pre-exposure prophylaxis (PrEP) and post-exposure prophylaxis (PEP).
The new policy will expand the donor pool, with potential to alleviate chronic blood shortages across the country that were exacerbated by the COVID-19 pandemic, says Dr. Vossoughi, who is also assistant professor of pathology and cell biology at Columbia University Vagelos College of Physicians and Surgeons.
As blood screening technology has improved over the years with support from scientific data, guidelines have shifted, she adds.
Donated blood is tested for a number of diseases including HIV, hepatitis B, and West Nile Virus.
“The testing has become very precise,” she says. “You’re more likely to get struck by lightning than to catch HIV from a transfusion, so the individual donor assessment coupled with the blood testing has made transfusion extraordinarily safe.”
The FDA recommendation comes as a result of data from the Assessing Donor Variability And New Concepts in Eligibility (ADVANCE) Study, which sought to determine if a donor history questionnaire based on individual risk would be just as effective as the three-month deferral period in reducing HIV risk in donated blood.
The new assessment approach will continue to maintain the safety of the blood supply, according to the FDA. It’s in line with similar policies in place in Canada and the United Kingdom.
While the updated guidelines may make way for more people being able to donate, there’s still work to be done to make blood donation more inclusive, says Dr. Vossoughi.
“We’ve done a lot, but we haven’t done enough,” she says. “This is very exciting and in the blood banking community, we want to keep going and pushing forward. The transfusion medicine community is actively engaged in this area of recruiting and retaining a diverse blood donor pool.”
Sarah Vossoughi, M.D., RN, is the medical director of apheresis and associate director of transfusion medicine and cellular therapy at NewYork-Presbyterian/Columbia University Irving Medical Center. She is also assistant professor of pathology and cell biology at Columbia University Vagelos College of Physicians and Surgeons. Prior to becoming a physician, Dr. Vossoughi served as a military officer, medical crew director, and trauma nurse in the U.S. Air Force in South Korea, Iraq, and Afghanistan, where she evacuated more than 900 troops out of combat zones, earning seven medals. Her research interests include hemovigilance, the processes that keep the blood supply safe, and risk management.
Additional Resources
Learn more on blood donation from the New York Blood Center.
Find out where you can donate or schedule a blood donation appointment.

